Is H7N9 influenza a ‘Stealth’ virus?
What we found: The bioinformatics team at EpiVax examined H7N9 (Shanghai 2013) sequence and found an unusually low number of T cell epitopes (see figure below). We predict that it will be difficult to make effective vaccines and low cost diagnostics for the newly emerging virus (also called H7N9/A/Shanghai/1/2013). Meaning – the new H7N9 may be a “stealth” virus that is able to fly under the immune system’s radar. And should the H7N9 “stealth virus” adapt itself for human-to-human transmission, it has serious potential for rapid expansion on a global scale.
What makes the new flu invisible to the immune system? The protein that is usually incorporated in vaccines known as HA (hemagglutinin) has fewer immune-stimulating T cell epitopes than many previously circulating strains of flu (see image). T cell epitopes have to be present in order for B cells to make high affinity and high titer antibodies. If antibody response is low, the virus could be transmitted faster and it may be harder to make effective vaccines.
What does that mean for diagnostic tests? Low T cell epitope content generally means that it is harder to make high-affinity antibodies, the type that are used to make low-cost diagnostic tests like ELISAs. While one rapid test for flu (based on PCR) is available, lacking a low cost rapid test, it could be harder to efficiently screen the expanding numbers of individuals that have already been exposed to active H7N9 cases (see here for the most recent count).
Is there another vaccine example that provides some evidence that this could be true? The analysis done by the EpiVax team of expert vaccine designers is consistent with reports by the CDC that previous H7 vaccines for similar viruses had low immunogenicity – (NEJM Article). Last season’s H3N2 was also predicted by EpiVax to be low immunogenicity, and epidemiological evidence of outbreaks among H3N2-vaccinated individuals confirms the prediction. Unless it is engineered for higher immunogenicity, a vaccine against H7N2 may have similar low efficacy as was seen with H3N2.
Other worrisome news: Experts in Japan report that the virus contains a signature that suggests transmission in mammals, and may also have some resistance to Tamiflu (two posts, see here and here). An epitope-based or epitope-adjuvanted vaccine might be more effective in this situation than one based only on the low immunogenicity HA. EpiVax has already evaluated the new H7N9 sequences and designed an epitope-based vaccine that could overcome this problem (more information here).
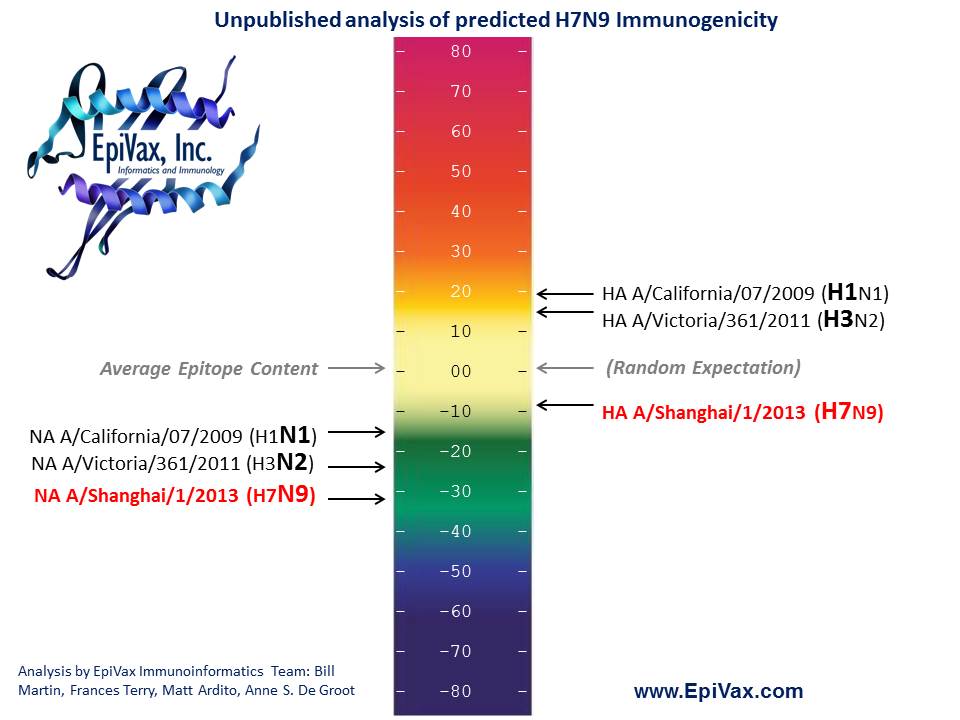
Unpublished analysis of predicted H7N9 Immunogenicity. Analysis by EpiVax Immunoinformatics Team: Bill Martin, Frances Terry, Matt Ardito, Anne S. De Groot.
EpiVax H7N9 Vaccine Effort is ongoing: Between April 6-8, 2013, EpiVax performed an extremely rapid analysis of the H7N9 vaccine sequence that is associated with an increasing number of deaths in Shanghai, China (see more at this link). Our H7N9 vaccine is based on the genome sequences provided on GISAID. It has both conserved (with other flu strain) and unique (to the novel strain) components. The conserved components could drive a memory response (by flu-specific T cells already be in the circulation). The unique T cell epitopes could help drive an antibody response that would be more specific for the emerging strain of H7N9 flu.
Previous proof of principle: The world was faced with a somewhat similar situation with pandemic H1N1, in 2009. At that time EpiVax experts correctly predicted that the exposure to, or vaccination by, seasonal influenza, would be protective. Our research was subsequently validated by Richard Webby, by Brian Schanen and Bill Warren. (Sanofi Pasteur) and others, as well as in our own laboratories. Epitopes that we predicted were conserved between in H1N1 2009 and seasonal flu were not only immunogenic in patients who had never seen Pandemic 2009, but were also protective against higher viral titers in the lungs of mice immunized with the epitopes and exposed to H1N1 pandemic (collaboration with Ted Ross, unpublished). Cross-protective information was widely distributed by Internet during the H1N1 pandemic, and later published. A similar ‘efficacy’ prediction was performed for Japanese encephalitis virus (Article). Additional studies that validate are available, please contact us here.
Existing Vaccine Efficacy: EpiVax is offering our tools to analyze existing H7N9 (and other H7) vaccines that are already available for potential cross-conservation at the T cell epitope level with the emerging H7N9 influenza sequences available from China. We understand that the CDC is at level 2 alert for influenza A (H7N9) due to the potential wide geographic spread of the outbreak. We are ready to help by analyzing and comparing existing vaccines with emerging H7N9 to provide a measure of predicted efficacy. It may not be necessary to make a NEW vaccine, saving many months and millions of dollars (and lives if this turns out to become a pandemic) and reduce the threat of economic standstill due to a pandemic influenza outbreak.
When EpiVax scientists performed a similar analysis of pandemic H1N1 in 2009, they correctly predicted that pandemic H1N1 would not cause severe disease in most individuals, a prediction that was subsequently validated in vitro and in vivo by many others. Unfortunately, the immunogenicity news is not so good for H7N9. We hope that the flu world will pay attention to the role of T cell epitopes in immune response to influenza, this time around.
Read more about H7N9 on our last two blogs Blog post 1, Blog post 2

